Disc herniation
Disc hernia: causes, symptoms and non-surgical treatment
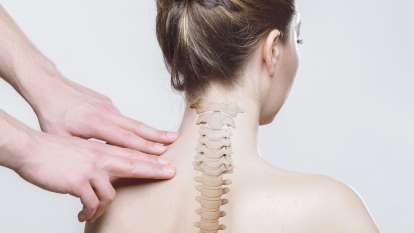
Disc hernia occurs most often in the lumbar area of the spine, being a form of discopathy. It is manifested by muscle contractions, chronic and sharp pain, numbness and tingling of the back, neck, arms and legs. Treatment is rare a surgical one, being preferred physiotherapy, kineto-therapy, acupuncture and natural remedies.
As a result of repeated physical trauma and long-lasting pressure in the spine, its discs are affected and discopathy occurs – which includes disc hernia and degenerative intervertebral disc disease. Disc hernia is manifested by pain and discomfort, caused by touching the nerves of the spine, as a result of the movement of discs that protect the vertebrae and absorb the shocks of daily activities: walking, lifting weights, twisting the body.
Most cases of disc hernia heal by themselves or with treatment, but the problem can recur. To protect your spine from shocks and pain, you need to consider simple and handy rules: the body must have a straight and standing posture, and when you sit down; weights rise from the knees, not forcing the back; extra pounds and smoking should be avoided.
What is disc hernia?
The bones that make up the spine (vertebrae) are amortized and stabilized by means of intervertebral discs. The discs consist of a pulpy, gelatinous nucleus, surrounded by a stronger, cartilaginous exterior. Disc hernia occurs when the outside cracks and a fragment of the nucleus of a disc is dislodged and pushed through this hole, pressing the nerves in the spine. This is how occurs the pain, which can be severe (but there are also people who do not have painful symptoms). A surgical intervention to treat the disc affected by hernia is necessary only in severe cases.
Types of disc hernia
Depending on the area where the dislocated disc is located, there are the following types of disc hernia:
- cervical: occurs in the upper part of the spine, at the first 7 vertebrae (C1-C7), close to the neck;
- thoracic: occurs in the following 12 vertebrae (T1-T12), in the chest area, being rare – only 1% of cases;
- lumbar: appears in the lower area of the spine, the following 5 vertebrae (L1-L5), close to the pelvis, being the most common type;
- sacral: occurs in the area of the last 5 vertebrae, located below the waist, including the coccyx.
Causes and risk factors
- a sedentary lifestyle;
- excess body weight/obesity;
- sitting in an incorrect position in the office chair;
- incorrect lifting of weights;
- wrong made physical exercise;
- trauma to the spine level (caused by excessive physical effort or an accident);
- excessively physical effort, motivated by occupation (people who have jobs that come with intense physical work have an increased risk of back problems);
- smoking (decreases the amount of oxygen that reaches the intervertebral discs and weakens them more quickly);
- aging (the material of the intervertebral discs degrades with age and the ligaments that hold them in place begin to weaken);
- genetic inheritance.
Symptoms
Typically, disc hernia is preceded by a single episode or a long history of back pain (which should send you to the doctor, because this disease can worsen very quickly). But depending on the position of the dislocated disc and the size of the hernia, symptoms vary greatly or may be completely absent.
These may include:
- chronic localized pain: these occur at the back of the neck, in the area of the shoulders, shoulder blades, collarbone and one of the arms (in the case of cervical hernia) or in the area of the back, buttocks, thighs and one of the legs (in the case of lumbar hernia); the pain may become acute when the patient sneezes, coughs, sits in certain positions, stands/sits, walks short distances; most often, lumbar disc hernia affects the sciatic nerve, causing so-called sciatica (manifested by pain, burns, numbness and tingling resembling an electric shock on one of the legs);
- difficulty or inability to turn your head and make sudden movements, inability to walk on peaks or heels;
- numbness, burning or tingling in areas related to the affected nerves, most often on one side of the body;
- painful muscle contractions/lumbago: seizures of the paravertebral muscles;
- muscle weakness: muscles served by the affected nerves are weakened and this can affect the ability to pick up objects and walk the sick person.
Complications of disc hernia
In rare cases, disc hernia can compress the entire vertebral canal, with all the nerves that control urination, for example. To avoid permanent weakness or paralysis, the patient will urgently need surgery. You must urgently see a doctor if you have the following symptoms:
- increasingly serious symptoms: pain, numbness, weakness so intense that it hinders your daily life;
- so-called "seat anesthesia": progressive loss of sensation in areas that would touch the horse's seat, if the patient were on a horse (inside the thighs, behind the legs, the area around the anus);
- cauda equine/ horsetail syndrome: serious effect of this condition, which is a neurosurgical emergency and manifested by symptoms in both lower limbs and incontinence (loss of control over the bladder and colon);
- permanent damage to the spinal cord: in very rare cases, the affected disc can compress the marrow and affect it irreparably.
Methods of treatment
Once you get to it, your specialist will give you the necessary assessments and tests, recommending a suitable treatment. But can you combat disc hernia by natural methods without resorting to medication and surgery? The answer is ”yes”. Specialists rarely recommend medical interventions in the case of the disc affected by hernia. Detected in due time, this condition can be treated by non-surgical therapy methods.
Rest and compresses
1-2 days of bed rest may be recommended by the doctor in case of the disc affected by hernia. These will give your back a rest period, in which the inflammation will decrease and the pain will decrease. Avoid sport and other physical activities involving lifting weights or bending your back. After a few days, get back on the move to keep your joints and muscles mobile. The pain can also be alleviated with cold or warm compresses placed on the area in question. You can alternate between the two temperatures (initially reduce inflammation using cold compresses, then switch to warm ones) or use the one that is more effective for you.
Kineto-therapy:
Kineto-therapy (recovery/medical gymnastics) is the therapy through motion and can include various accessories (a medicinal ball, for example). On the advice of the physiotherapist, a personalized exercise program is followed by the patient with the affected disc, the results being carefully monitored. Exercises with various degrees of complexity are designed to reduce the pressure that the disc exerts on the nerve, to tone the back muscles, stabilize the spine and eliminate pain from the landscape.
Physiotherapy:
Physiotherapy is a method of treatment that combats pain by appealing to physical agents: mechanical or magnetic waves, heat, light, electricity. A physiotherapist can recommend various methods to treat disc hernia:
- therapeutic massage: relieves short-term pain, improves circulation and helps to synovial fluid secretion (which is important speaking of joint restoration); there are over 100 massage techniques, the specialist therapist being the right person to find the right method for you;
- thermotherapy: the use of heat or low temperature for therapeutic purposes to relieve the patient's discomfort;
- TECAR therapy: using electromagnetic energy, stimulates the body's natural healing process, improving pain;
- electrostimulation: reproduces natural muscle contraction with the help of electric current;
- hydrotherapy: special exercises, which the patient does in a pool with warm water;
- Laser therapy: the use of a low-intensity laser wave (less than 500 mW) is a non-invasive procedure that eliminates pain, relaxes muscles and stimulates tissues;
- ultrasound: have analgesic, vasodilator, muscles relaxant and acceleration effect of the healing process of tissues;
- magneto-therapy: magnetic fields have an effect on painful points and mobility is restored;
- elongation: a process by which a spinal decompression is performed, the patient's spine being stretched and its segments being realigned.
- inversion bank: is a very good and safe method of natural elongation. If we imagine the column as a permanent compressed resort due to various factors that overload it, we will understand how effective decompression is. Basically, the inversion bank allows us to rotate the body degree up to 180 degrees; if the hernia is cervical and the bank rotated to 180 degrees, practically an elongation will occur given by the weight of the head.
Alternative methods
- chiro-practice: this alternative therapy consists in manual correction of the spine by the chiropractor, in order to de-stress it; column handling may be effective in keeping back pain at the distance for at least one month;
- acupuncture: this component of traditional Chinese medicine can reduce inflammation and relax muscles, reducing chronic back and neck pain; extremely thin needles are inserted at certain points on the meridians of the body and left to act for 20-40 minutes;
- acupressure/ acupressure: similar to acupuncture, this therapeutic method consists of pressing or massaging certain points on the surface of the skin, which have special biological activity;
- yoga: the old practice popularized by Indians can reduce back pain through the combination of light exercise, breathing and meditation.
Natural remedies:
- turmeric can reduce inflammation and pain in sciatica, due to the content of curcumin; can be consumed as capsules or dry extract; 300 mg is recommended, 3 times/day; alternatively, you can take curcumin supplements (200-5,000 mg/day); consume them both in combination with black pepper, which significantly increases the absorption of this active substance which gives turmeric its intense color;
- ginger contains 14 bioactive compounds, with gingerol being analgesic and anti-inflammatory, helping to manage pain and reduce inflammation; can be consumed as such or as a dietary supplement (powder/capsules);
- comfrey may be beneficial for the relief of low back pain; try applying compresses with comfrey for 5 days in a row.
- against sciatica pain, internal infusions of elderflowers and primrose flowers, decoctions from angelic roots and willow bark, pine bud syrup or willow bark macerate and wine can be attempted;
- externally, the sciatic nerve affected by the disc hernia can be treated using: warm poultices (with St John's wort grass; garden ruta; a mixture of horseradish roots, homage and comfrey, thyme, shepherd's purse, hellebore, ground seeds of black mustard, grated potato, sliced onion and cabbage leaves), massage with hot pepper tincture, wild chestnuts, lilies, dedita, knapweed, bay and Swedish bitter or with a mixture of juniper oil, lavender, chamomile, mint, willow, St John's wort, garlic and turpentine/rosemary oil essence;
- pains can be reduced by warm sitting and foot baths, the temperature of which will be progressively increased: in water add decoction of hay flowers, elderflower, arnica, fern, hellebore, nettle, black mustard, celandine and a few drops of mint oil; in addition, during the bath drink 1-2 cups with lemon juice diluted with water;
- a marigold ointment and a piece of wolf plant - filled material may be applied to the painful area;
- a diet rich in animal collagen, obtained by boiling bones in soups and consuming them; 2-3 servings/ day is recommended;
- MSM, Glucosamine and Condroitin supplements also contribute to joint repair; they contain hyaluronic acid and sulfur, a combination that helps cartilage, lubricates and ensures their elasticity and shock absorption capacity.
Medicines:
Anti-inflammatory drugs, analgesics and pills intended for muscle relaxation may be recommended by the specialist in combination with physiotherapy. In addition, the patient may be prescribed cortisone injections in the area of the affected nerves.
Surgical treatment:
Recommended only in severe cases of disc hernia, certain surgical interventions can repair the problem. The specialist may recommend chemo-nucleolysis (injecting an enzyme into the problem disc to dissolve its nucleus), (micro)disectomy (partial/ total removal of the affected disc), lumbar / cervical laminectomy (by which the pressure on the affected nerve is reduced) or artificial replacement of the disc (with a plastic or metal one, which will stabilize the spine).
How can you prevent disc hernia?
We know that prevention is always easier than treatment and in the case of the affected disc the former is all the more important because this condition causes constant pain, which not everyone can get rid of by conventional methods. And no one wants to get to the knife, does it? Discover below the elements that can help you avoid the appearance of such a hernia:
- do sports regularly: strengthening the muscles of the back, abdomen and legs stabilizes and supports the spine;
- avoid sedentary behavior at work: do not sit down for hours in a chair, get up periodically and move around the desk, go out for a breath of air, or sit down with a colleague in the hallway, standing up;
- keep your weight to your height: excess pounds, overweight or obesity put more pressure on the intervertebral discs and the risk of herniated discs increases;
- dose your physical effort correctly: be careful how you lift and move very heavy objects (as weightlifters do, bend your knees when you lift them, not your waist);
- keep your back straight: a proper posture of the body will reduce the pressure on your spine; If you need to stand for many hours, rest one foot on a box or a low seat to remove the pressure on your back;
- quit smoking: toxins in cigarettes affect the proper oxygenation of the spine and cigarettes cause hardening of the arteries, affecting your intervertebral discs
Did you know that...?
- In general, the term "hernia" refer to the movement of an organ from its natural cavity?
- Does disc hernia occur more often at men than at women?
- The spine consists of 33 individual bones, which are placed on top of each other and which are called vertebrae? The first 24 are separated by intervertebral discs, which constitute natural shock absorbers?
- Disc hernia can occur in any area of the spine?
- Treatment based on modification of activities that cause pain, kineto-therapy and/or administration of anti-inflammatory and analgesics can reduce the symptoms of the disc affected by hernia within a few days or weeks?
Comments